A North West London case study

Background
It is well-evidenced that avoidable intrapartum brain injury can have devastating consequences for babies and their families, along with lifetime impacts for health and care services. The Avoiding Brain Injury in Childbirth (ABC) programme has its origins in a call for action by the Treasury in 2018 on the costs of litigation associated with avoidable brain injury.
Through national implementation, the ABC programme aims to strengthen clinical practice and improve communication and care for women and families, leading to better outcomes and experiences.
Project aims
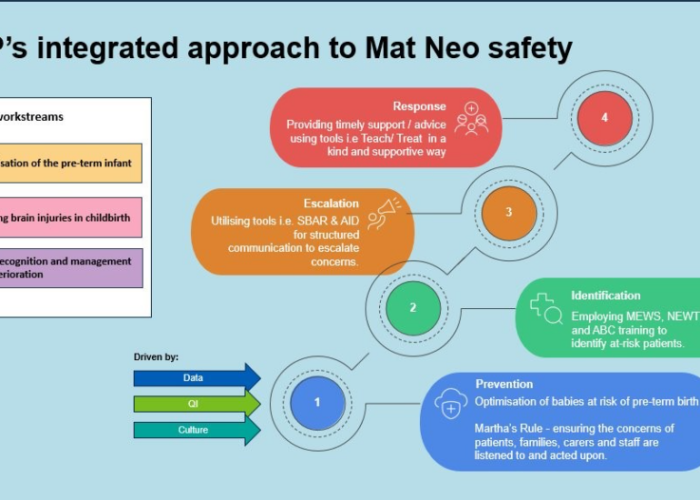
The project will help maternity staff improve clinical practice of two significant contributors to avoidable brain injury in childbirth:
1. The detection and response to suspected intrapartum fetal deterioration (IFD)
2. The management of the obstetric emergency of impacted fetal head (IFH) at caesarean birth
ICHP, as the steward of the North West London (NWL) Patient Safety Collaborative (PSC), has been commissioned to support each maternity site in NWL to deliver the ABC programme, with IFH being delivered in 2025-26, and IFD to be delivered in 2026-27.
To date, we’ve focused on delivering ‘Train the Trainers’ sessions, focused on managing IFH at caesarean birth to maternity teams across NWL, helping to standardise clinical practice and build confidence in recognising IFH as an obstetric emergency.
The key aims of this arm of the ABC programme are:
- Reducing variation in obstetric emergency response for IFH between trusts
- Embedding evidence‑based national guidelines and training into everyday maternity practice
- Improving safety for birthing people and babies by reducing the risk of avoidable brain injury.
This project is associated with the Maternal & Neonatal space & aligned with the government’s aim to reduce the unwarranted variation in outcomes across England.
By narrowing this gap, it will support the majority of maternity units to achieve outcomes comparable to those currently attained by the highest-performing 20%. The reduction in the number of children born with Cerebral Palsy could reduce litigation costs by £860 million – £1.4 billion per year.
Method
From the outset, our approach to the ABC programme focused on ensuring that each trust received a practical, context‑specific learning experience that strengthened their capability to manage impacted fetal head. We began by working closely with local training leads to understand existing training models, identify variation in practice, and understand where IFH training could add the greatest value.
Building on this foundation, we delivered Tier 2 ‘Train the Trainer’ sessions across NWL, bringing obstetricians and midwives together to explore updated approaches to IFH management and to familiarise themselves with the new clinical algorithms. These sessions prioritised multidisciplinary discussion, and confidence‑building in recognising IFH as a time‑critical obstetric emergency.
By investing time in building relationships with individual trust teams and understanding local context, we created strong local ownership of the programme. This collaborative approach has generated system‑wide enthusiasm for adoption and spread, supporting more consistent implementation across maternity services.
Impact
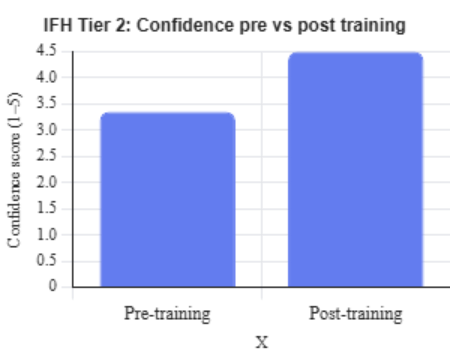
The programme has already started to reshape the management of IFH across NWL. With T2 training delivered in three trusts, and the fourth soon to follow, we’ve consistently received strong engagement and enthusiasm from staff. The training clearly resonated, with average confidence increasing from 3.35 pre‑training to 4.5 post‑training, and participants consistently valuing the hands‑on format.
Additionally, we’ve shared resources created by ICHP’s Clinical Faculty nationally, via NHS Futures, contributing to the culture of shared learning the PSCs have fostered, and showing our commitment to scaling and spreading good practice. This includes a mannikin set up video.
By creating more consistent practice across the region, we’re laying out the foundation for longer‑term improvements in maternal and neonatal outcomes. We have also invited peer review from other HINs to quality assure our training delivery against the national standard.
“The team found it very helpful and engaging. They particularly valued the opportunity to practice delivering an impacted fetal head, including vaginal disimpaction and breech delivery via caesarean section. The session was very interesting, and the practical elements supported learning and confidence in managing these complex scenarios.”
– Lead Midwife for Practice Development
Chelsea & Westminster NHS Foundation Trust
Scalability and next steps
Over the coming months, we’ll be supporting each trust to deliver the new IFH training through their own internal PDM and education teams, ensuring high-fidelity and confidence in the delivery of the training remains high. Alongside this, we’ll be working with trusts to formalise IFH management as a recognised obstetric emergency by developing SOPs that can be adopted across maternity units.
A major step will also involve collaborating with digital and clinical teams to integrate the IFH proforma into existing caesarean section documentation within trusts’ electronic patient record systems. This will help build the data we have on IFH cases and help us review the effectiveness of the IFH management across NWL.
Partners
- NWL maternity Trusts (The Hillingdon Hospitals NHS Foundation Trust, London North West University Healthcare NHS Trust, Chelsea and Westminster Hospital NHS Foundation trust, and Imperial College Healthcare NHS Trust).
- NHS England, London health innovation networks (HINs), Practice Delivery Midwifery Leads, Obstetricians, and simulation training teams across the region.
- ICHP’s Clinical Faculty providing leadership in spread and adoption, implementation support, and programme coordination.
ICHP, as part of our Patient Safety Collaborative commission from NHS England, has contributed expertise in the project design, implementation, stakeholder relationships and collaboration, programme evaluation, Trust engagement and training delivery
Our clinical faculty has contributed their clinical expertise and experience in working within the NWL system, to build relationships across NWL and deliver the training of IFH.
Together we have worked with Hillingdon Hospitals in creating a standard operating procedure (SOP) for IFH and with the Acute Provider Collaborative on Cerner implementation, ensuring IFH is recognised as an emergency on the recording paperwork and thereby creating conditions for future evaluation of outcomes.
The Cerner piece is evidence of the NWL appetite for embedding this within their routine workflows.
The IFH SOP is currently being developed for NWL wide use.
Our thanks go to the maternity educators, obstetric leads, and simulation teams across all participating trusts, whose insight and enthusiasm have shaped every stage of the programme. We also recognise NWL’s ABC clinical faculty for guiding the programme and contributing their time and expertise to the progress of this programme.
Want to learn more about the ABC workstream? Get in touch with our team
Dr Ololade Obadare, Project Lead – ololade.obadare@imperialcollegehealthpartners.com
Dr Millicent Nwandison, Clinical Faculty – m.nwandison@nhs.net
Isabella Luxton, Clinical Faculty – isabella.luxton@nhs.net
Fazeela Chharawala, MatNeo Lead – fazeela.chharawala@imperialcollegehealthpartners.com