Clare Thomson, Innovation Lead for the North West London mission-led approach to Cardiovascular Disease, shares why detection of the disease is a strategic priority for our region, and how crucial and vital it is in accelerating it.
Cardiovascular Disease (CVD) remains the leading cause of premature death in the UK, responsible for one in four lives lost. In North West London (NWL) alone:
- Over a million adults live with high cholesterol, with up to 900,00 unaware and undiagnosed
- Over 300,000 residents have high blood pressure,
- Up to 425,000 adults in NWL may have undiagnosed hypertension
- Around 13,000 adults are likely to have undiagnosed atrial fibrillation (AF).
Behind each of those numbers are families whose lives could be transformed, or even saved, by acting earlier.
That’s why, as the innovation partner for NWL, Imperial College Health Partners (ICHP) is working with the NHS, industry, and communities to put early detection at the heart of our region’s mission-led approach to CVD. We see this as one of the most urgent and impactful areas where innovation can shift the dial – not only saving lives but reducing inequalities and easing pressure on frontline services.
And our ambition is bold. As part of NWL’s mission-led approach to CVD, we aim to have prevented 25% of heart attacks and strokes in our region by 2029, whilst actively addressing health inequalities in CVD.
And to achieve that, innovation isn’t optional – it’s essential.
Why are we focusing on detection?
By detecting not just CVD but the risk of CVD earlier – through high cholesterol, high blood pressure, HbA1c (diabetes), atrial fibrillation, and other risk factors – we can prevent thousands of avoidable CVD events.
The government’s three shifts for health make this both a local and a national priority:
- From treatment to prevention: The NHS Long Term Plan and Core20PLUS5 both call for stronger prevention of CVD as a key lever to reduce inequalities.
- From hospital to community: From workplaces to community venues, moving beyond GP surgeries expands reach and makes screening more accessible.
- From analogue to digital: Digital point-of-care innovations, like PocDoc, mean results and tailored advice can be delivered in minutes, without needing a lab or GP appointment.
What does innovation look like in the detection space?
One of the most promising solutions we’ve tested locally is PocDoc – identified through our Innovation Exchange function thanks to it’s alignment with our region’s Mission-led approach to improving CVD care.
Their easy-to-use, rapid testing kits deliver a complete picture of heart health (including cholesterol, heart age and overall CVD risk level) in under 10 minutes, and can be used outside of clinical settings. From workplaces to community hubs, they make early detection accessible and convenient. Their goal? To help identify those at highest risk of CVD and ensure they receive the right treatment.
What have we learned from local testing?
In 2025, we’ve tested PocDoc’s innovative approach to CVD detection in both workplace and community settings. Two recent pilots, delivered in partnership with NWL ICB and PocDoc, offer valuable lessons:
1. Workplace-based heart health checks for NHS staff
- 31 staff members participated in point-of-care CVD screening afternoon using the PocDoc platform in the NHS NWL ICB offices
- 45% of participants had never had a cholesterol test before
- Only 23% had undergone testing in the past year, and a further 29% had been tested within the last five years
- 39% were found to have high cholesterol, as well as raised triglyceride levels (excess of fat in the blood).
- Lifestyle or dietary recommendations were made in 33% of cases.
- Staff overwhelmingly preferred workplace-based digital screening, with 95% of participants saying it was more convenient than a GP visit.
- The pilot demonstrated that unmet screening needs exist even among NHS staff, and that digital workplace screening is feasible, scalable and well received.
Get in touch to read our full evaluation
2. Community heart checks in Harefield
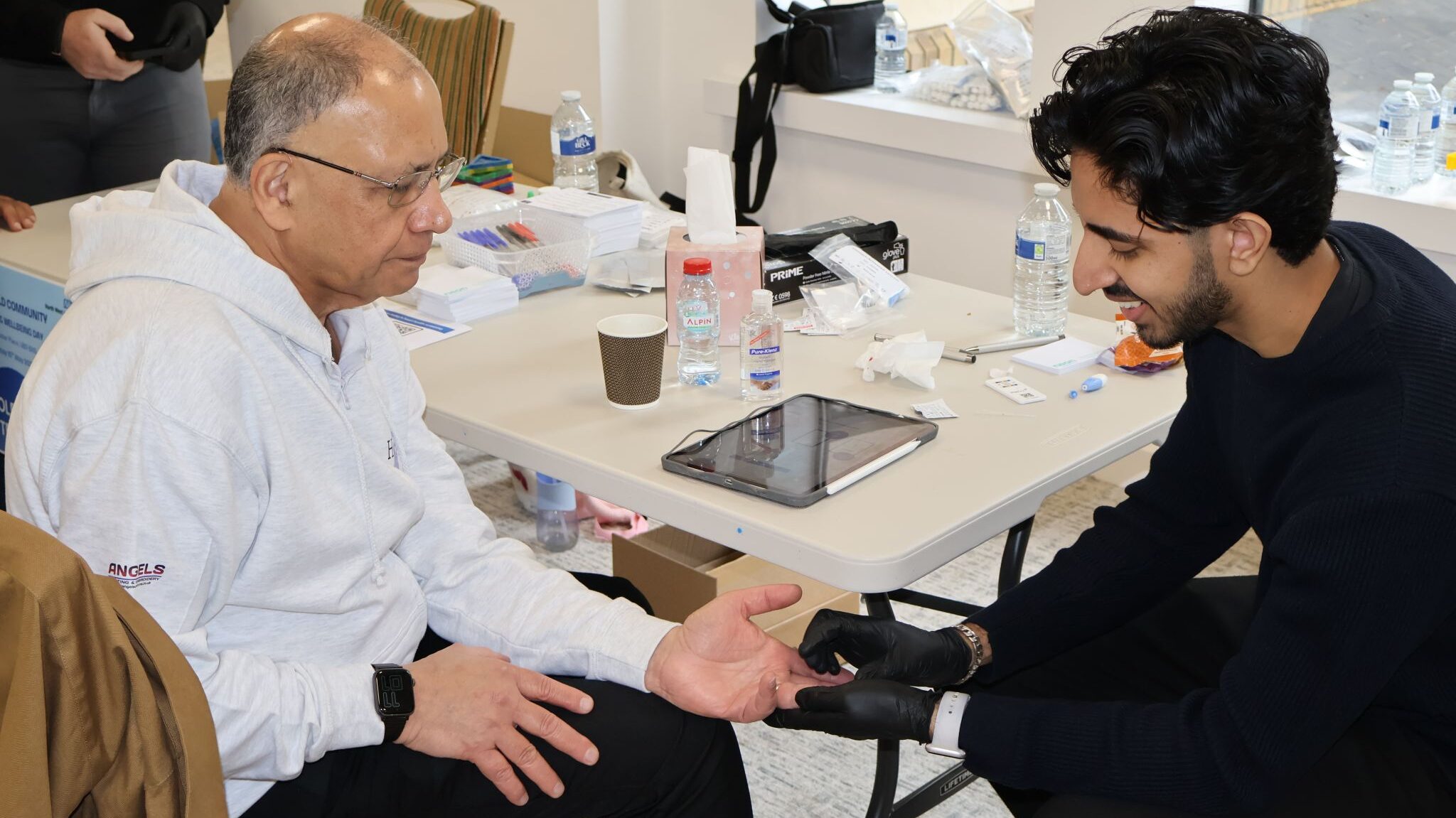
- We piloted PocDoc at a community-based health and wellbeing event (which CVD screening was part of)in Harefield, engaging 31 residents.
- 32% of residents screened had never had cholesterol checks previously.
- 13% were identified as high CVD risk (QRISK ≥10%).
- 25% had high cholesterol and19% raised triglycerides,
- The event reached a higher proportion of Asian and minority ethnic residents (58%) compared with local census figures.
- 34% of participants were advised to follow up with their GP.
- Residents described the process as “very easy, excellent and slick,” with many reporting increased motivation to improve their lifestyle.
- Volunteer GPs valued the immediate results for more meaningful advice conversations.
Get in touch to read our full evaluation
Together, these pilots demonstrate that meeting people where they are, whether in workplaces, libraries, or community centres, makes prevention feasible, accessible and effective.
What does this mean for the system?
Early detection not only delivers better outcomes for individuals, it also has system-wide benefits:
- Reduced GP burden: rapid tests in community or workplace settings free up GP time.
- Addressing health inequalities: targeting underserved communities ensures prevention reaches those most at risk.
- Economic value: preventing strokes and heart attacks saves significant costs in acute and long-term care .We anticipate that community-testing in this way is likely to prevent a minimum of 2.6 CVD events per cohort, totalling savings of over £46k (based on a cost to the NHS per stroke of +£17k).
- Scalability: Although this innovation is relatively low cost and can be supported by non-clinical staff, as well as clinical staff, long-term funding discussions needs to happen with a variety of stakeholders to ensure sustainability and scalability.
So, what now?
Projects like PocDoc show that innovation is not a “nice-to-have”, it’s essential in achieving this scale of change. The lesson from these projects are clear – when we move detection beyond GP surgeries and into spaces where people live and work, earlier detection becomes practical, accessible and impactful.
We’re now looking at how we expand this project further. We’re working closely with the NWL Health Equity team on a community in-reach model and what an offer for CVD testing at NHS workplaces across NWL could look like. Why? To both improve staff health and reduce costs. We project that by implementing and scaling this approach at one trust alone, we could prevent up to 91 cases of CVD and save over £25,000 by avoiding agency costs linked to days lost to staff CVD-related sickness.
Via this system-wide approach to CVD detection, we’ll continue to convene innovators, clinicians, leaders, and communities, to detect earlier so we can act faster and save lives.
Work with us
If you are an innovator with solutions that can support early detection, prevention, or management of CVD, we want to hear from you. Get in touch at innovators@imperialcollegehealthpartners.com.
Work in CVD in NWL and interested in testing innovative solutions? Drop us a line at clare.thomson@imperialcollegehealthpartners.com.



